Disease Overview
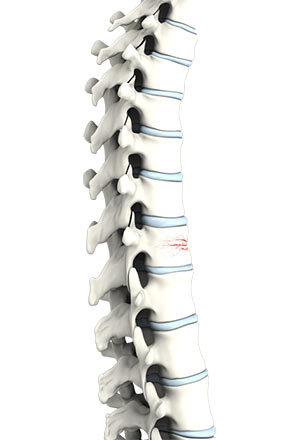
Osteoporosis is a “silent” disease characterised by weakening of bones, making them more susceptible to fractures, typically in the hip and spine. Elderly people and especially post-menopausal women are at greater risk of developing osteoporosis.
The mid to lower back area of the spine is mainly involved in weight-bearing, making these regions of spine more prone to collapse when bone weakness is present. This can lead to spinal (vertebral) compression fractures. Many of these vertebral compression fractures occur by minimal trauma or by no trauma at all. They can even occur while performing simple activities, like bending or twisting.
Symptoms of Spine Osteoporosis
Symptoms range from severe pain in the back, arms and legs to no pain at all. You may believe that your back pain is just a part of ageing, letting these vertebral compression fractures go undiagnosed. However, a single vertebral fracture significantly increases your risk of further fractures. When multiple fractures occur, it causes the spine to become rounded and bend forward, resulting in loss of height and a hunchback appearance. This forward curvature of the spine negatively affects the quality of life and makes it more difficult for you to breathe, eat, walk or sleep. Vertebral compression fractures can also occur from conditions such as a metastatic tumour, multiple myeloma, and vertebral haemangioma.
What is Vertebroplasty?
Vertebroplasty is a minimally invasive procedure performed to reduce or eliminate pain caused by a vertebral compression fracture. It stabilises the fracture and prevents further collapse of the vertebra, averting deformity.
Contraindications of Vertebroplasty
The procedure cannot be performed under the following situations:
- A compression fracture is stable and does not cause any pain
- A fractured fragment or tumour is present in the spinal canal
- Presence of a bone infection or bleeding disorder
Vertebroplasty Procedure
- The vertebroplasty procedure involves the injection of bone cement into the fractured vertebra under high pressure.
- The procedure is performed under general or local anaesthesia. You will be lying face down on the operating table.
- Your doctor will make a very small 1/2-inch incision on the skin over the fracture site. Under live X-ray guidance, a hollow needle called a trocar is introduced through the back and positioned within the fractured vertebrae.
- Next, bone cement is injected into the area through the trocar under high pressure.
- After the vertebral body is filled completely with the bone cement, the needle is withdrawn before the cement hardens.
X-rays or CT scans may be taken to confirm the effective spread of the bone cement into the fractured vertebra. The skin incision is closed using steri-strips.
Risks and Complications of Vertebroplasty
As with any surgery, some risks can occur. General complications include bleeding, infection, blood clots and reactions to anaesthesia. The specific complications following a thoracic vertebroplasty include leakage of the bone cement into the surrounding soft tissues or veins, and damage to the spinal cord or spinal nerves, leading to numbness or paralysis.
Related Topics:
- Minimally Invasive Spinal Surgery
- Advanced Pain Management
- Laser Disc Surgery (PLDD)
- Spinal Epiduroscopy (Endoscopy)
- Regenerative and Stem Cell Service
- Non-Surgical and Rehabilitation Service
- Back Pain
- Kyphoplasty
- Spinal Fusion
- Spinal Stenosis
- Radiofrequency Denervation (Radiofrequency Ablation)
- Spinal Ozone Therapy
- Spinal Injections
- Vertebroplasty
- Physiotherapy
- Osteopathy